XXXI Congresso Nazionale Intergruppo Melanoma Italiano (IMI)
2025: XXXI Congresso Nazionale Intergruppo Melanoma Italiano (IMI)
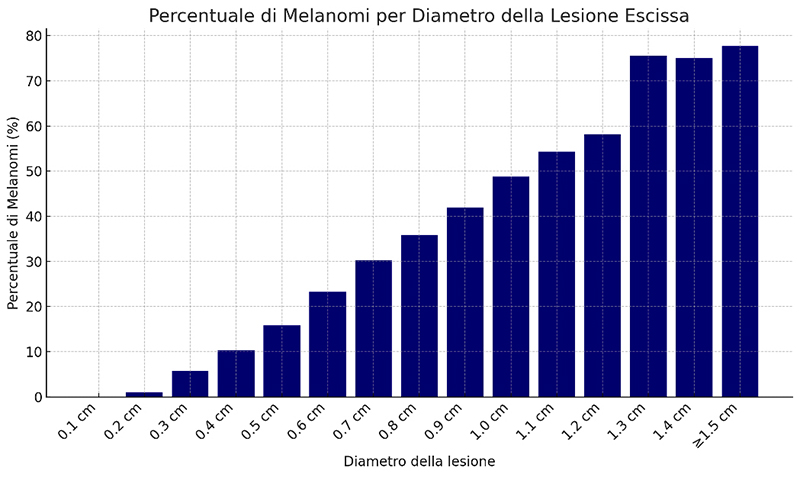
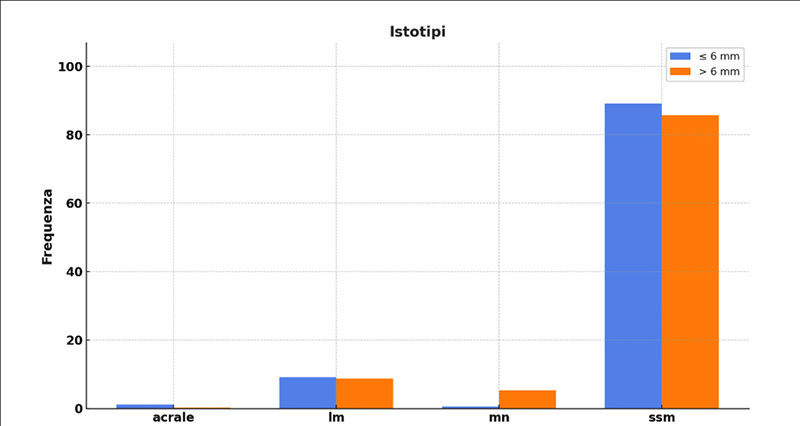
07 | Early diagnosis of melanoma in the era of non-invasive imaging: histopathological confirmation of malignancy vs. clinical suspicion. a retrospective study of 2240 patients
Giovanni Cecchi1, Gabriella Perillo1, Federica Fazzari1, Virginia Marabini2, Biancamaria Zuccaro1, Vincenzo De Giorgi1 | 1Dipartimento di Scienze della Salute, Sezione di Dermatologia, Università di Firenze; 2Dipartimento di Scienze della Salute, Università di Firenze, Italy.

Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 11 December 2025
289
Views
0
Downloads